Levofloxacin Drug: Indication, Dosage, Precaution, Side Effect , Storage, Category Type and corresponding Brands - www.genericdrugscan.com
Levofloxacin
Drug Status in USA : ApprovedDrug Status in Canada : Approved
pronunciation
pronounced as (lee voe flox' a sin)
Why is this medication prescribed?
Levofloxacin is used to treat certain infections such as pneumonia, chronic bronchitis and sinus, urinary tract, kidney, prostate (a male reproductive gland), and skin infections. Levofloxacin is also used to prevent anthrax (a serious infection that may be spread on purpose as part of a bioterror attack) in people who may have been exposed to anthrax germs in the air. Levofloxacin is in a class of antibiotics called fluoroquinolones. It works by killing bacteria that cause infections. Antibiotics will not work for colds, flu, or other viral infections.
How should this medicine be used?
Levofloxacin comes as a tablet and a solution (liquid) to take by mouth. It is usually taken once a day. The length of your treatment depends on the type of infection you have. Your doctor will tell you how long to take levofloxacin. The tablet may be taken with or without food. The solution should be taken 1 hour before or 2 hours after eating. Take levofloxacin at around the same time every day. Follow the directions on your prescription label carefully, and ask your doctor or pharmacist to explain any part you do not understand. Take levofloxacin exactly as directed. Do not take more or less of it or take it more often than prescribed by your doctor.
You should begin to feel better during the first few days of treatment with levofloxacin. If your symptoms do not improve or if they get worse, call your doctor.
Take levofloxacin until you finish the prescription, even if you feel better. Do not stop taking levofloxacin without talking to your doctor unless you experience certain serious side effects listed in the IMPORTANT WARNING or SIDE EFFECTS sections. If you stop taking levofloxacin too soon or skip doses, your infection may not be completely treated and the bacteria may become resistant to antibiotics.
What are the precautions to be followed?
Before taking levofloxacin,- tell your doctor and pharmacist if you are allergic or have had a severe reaction to levofloxacin; any other quinolone or fluoroquinolone antibiotic such as ciprofloxacin (Cipro), gatifloxacin (Tequin) (not available in the U.S.), gemifloxacin (Factive), lomefloxacin (Maxaquin) (not available in the U.S.), moxifloxacin (Avelox), nalidixic acid (NegGram), norfloxacin (Noroxin), ofloxacin (Floxin), and sparfloxacin (Zagam) (not available in the U.S.): or any other medications, or if you are allergic to any of the ingredients in levofloxacin tablets or solution. Ask your pharmacist or check the Medication Guide for a list of the ingredients.
- tell your doctor and pharmacist what other prescription and nonprescription medications, vitamins, nutritional supplements, and herbal products you are taking or plan to take. Be sure to mention the medications listed in the IMPORTANT WARNING section and any of the following: anticoagulants ('blood thinners') such as warfarin (Coumadin, Jantoven); certain antidepressants; antipsychotics (medications to treat mental illness); cyclosporine (Gengraf, Neoral, Sandimmune); diuretics ('water pills'); insulin; oral medications for diabetes such as glyburide (DiaBeta, in Glucovance, Micronase, others); certain medications for irregular heartbeat such as amiodarone (Cordarone), procainamide (Procanbid), quinidine, and sotalol (Betapace, Betapace AF, Sorine); nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen (Advil, Motrin, others) and naproxen (Aleve, Naprosyn, others); tacrolimus (Prograf); or theophylline (Elixophyllin, Theo-24, Uniphyl, others). Your doctor may need to change the doses of your medications or monitor you carefully for side effects.
- if you are taking antacids containing aluminum hydroxide or magnesium hydroxide (Maalox, Mylanta, Tums, others), didanosine (Videx), sucralfate (Carafate), or vitamin or mineral supplements that contain iron or zinc, take these medications 2 hours before or after you take levofloxacin.
- tell your doctor if you or anyone in your family has or has ever had a prolonged QT interval (a rare heart problem that may cause irregular heartbeat, fainting, or sudden death) or an irregular heartbeat, and if you have or have ever had nerve problems; a low level of potassium in your blood; a slow heartbeat; cerebral arteriosclerosis (narrowing of blood vessels in or near the brain that can lead to stroke or mini-stroke); seizures; chest pain; or liver disease.
- tell your doctor if you are pregnant, plan to become pregnant, or are breast-feeding. If you become pregnant while taking levofloxacin, call your doctor.
- you should know that levofloxacin may cause confusion, dizziness, lightheadedness, and tiredness. Do not drive a car, operate machinery, or participate in activities requiring alertness or coordination until you know how this medication affects you.
- plan to avoid unnecessary or prolonged exposure to sunlight or ultraviolet light (tanning beds and sunlamps) and to wear protective clothing, sunglasses, and sunscreen. Levofloxacin may make your skin sensitive to sunlight or ultraviolet light. If your skin becomes reddened, swollen, or blistered, like a bad sunburn, call your doctor.
What are possible side effects of this medication ?
Levofloxacin may cause side effects. Tell your doctor if any of these symptoms are severe or do not go away:- nausea
- vomiting
- diarrhea
- stomach pain
- constipation
- heartburn
- headache
- vaginal itching and/or discharge
- severe diarrhea (watery or bloody stools) that may occur with or without fever and stomach cramps (may occur up to 2 months or more after your treatment)
- dizziness
- confusion
- nervousness
- restlessness
- anxiety
- not trusting others or feeling that others want to hurt you
- difficulty falling asleep or staying asleep
- nightmares or abnormal dreams
- hallucinations (seeing things or hearing voices that do not exist)
- depression
- thoughts about dying or killing yourself
- uncontrollable shaking of a part of the body
- rash
- hives
- itching
- peeling or blistering of the skin
- fever
- swelling of the eyes, face, mouth. lips, tongue, throat, hands, feet, ankles or lower legs
- hoarseness
- difficulty breathing or swallowing
- fast heartbeat
- fainting
- loss of consciousness
- yellowing of the skin or eyes
- dark urine
- decreased urination
- seizures
- unusual bruising or bleeding
- joint or muscle pain
Levofloxacin may cause problems with bones, joints, and tissues around joints in children. Levofloxacin should not normally be given to children younger than 18 years of age unless they have been exposed to anthrax in the air. If your doctor prescribes levofloxacin for your child, be sure to tell the doctor if your child has or has ever had joint-related problems. Call your doctor if your child develops joint problems, such as pain or swelling, while taking levofloxacin or after treatment with levofloxacin.
Levofloxacin may cause nerve damage that may not go away even after you stop taking levofloxacin. This damage may occur soon after you begin taking levofloxacin. If you experience any of the following symptoms, call your doctor immediately: numbness, tingling, pain, or burning in the arms or legs; or a change in your ability to feel light touch, pain, heat, or cold. If you experience these symptoms, do not take any more levofloxacin until you talk to your doctor. Your doctor may prescribe a different antibiotic for you to take instead of levofloxacin.
Talk to your doctor about the risks of taking levofloxacin or giving levofloxacin to your child.
Levofloxacin may cause other side effects. Call your doctor if you have any unusual problems while taking this medication.
How to store the medication and dispose it of after its use later?
Keep this medication in the container it came in, tightly closed, and out of reach of children. Store it at room temperature and away from excess heat and moisture (not in the bathroom). Throw away any medication that is outdated or no longer needed. Talk to your pharmacist about the proper disposal of your medication.
Drug Category/Class
- Anti-Bacterial Agents
- Anti-Infective Agents, Urinary
- Topoisomerase II Inhibitors
- Fluoroquinolones
- Quinolones
- Ophthalmologicals
- Sensory Organs
- Alimentary Tract and Metabolism
- Antibacterials for Systemic Use
- Antiinfectives for Systemic Use
- Antiinfectives
- Drugs for Peptic Ulcer and Gastro-Oesophageal Reflux Disease (Gord)
- Drugs for Acid Related Disorders
- Quinolone Antibacter
| Prescribed | For the treatment of bacterial conjunctivitis caused by susceptible strains of the following organisms: Corynebacterium species, Staphylo... |
| Weight : | 361.3675 |
| Structure | Levofloxacin |
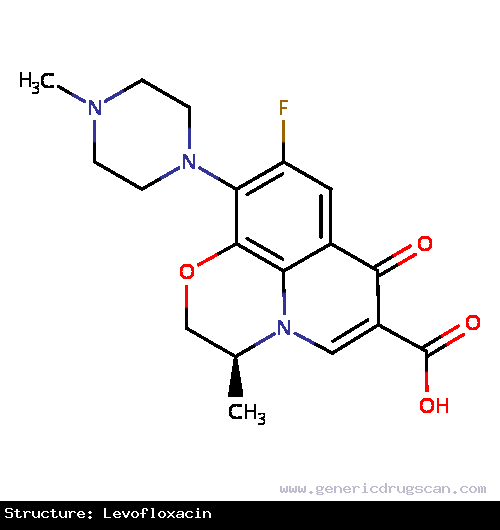 | |
| Formula | C18H20FN3O4 |
Levofloxacin has 904 Brands listed
Search Generic Drugs alphabetically
